Medication mismanagement costs the United States healthcare system one in every six dollars. In the arduous trek to value-based care, medication optimization is the mountain the U.S. healthcare system hasn’t yet been able to scale. Costs associated with drug-related problems only threaten to grow every single year.
A solution to medication mismanagement would help fix a more than $500 billion-dollar problem and enable millions of people to live their healthiest lives. According to the Journal of the American Geriatrics Society, hospital utilization would decrease, impacting health outcomes and cost of care. However, current medication therapy management processes are difficult to deliver at scale as a result of the sheer workforce volume needed to sift through patients' medication data, stratify patient risk, and reach out personally to counsel each individual about their use of medication.
At Arine, we believe medication mismanagement is solvable. We are on a mission to ensure that millions of Americans receive the safest, most effective, and most appropriate treatment for their unique and evolving healthcare needs. We recently raised $11 million in our Series A round, and we’re putting our funding to use accelerating our AI-driven medication optimization platform that personalizes medication management and delivers outcomes at scale. Here’s how we do it:
Medication Optimization Through Whole-Person Care
Comprehensive medication management (CMM) that doesn’t consider the whole person can hardly be called comprehensive. Many medication management processes focus only on disparate parts of a person’s care such as the medications they take, polychronic conditions, and the other aspects of a person’s circumstances and environment that impact their health and well-being. Without a full picture, care teams can’t deliver care that will impact the individual’s health and improve patient outcomes and costs for a population overall.
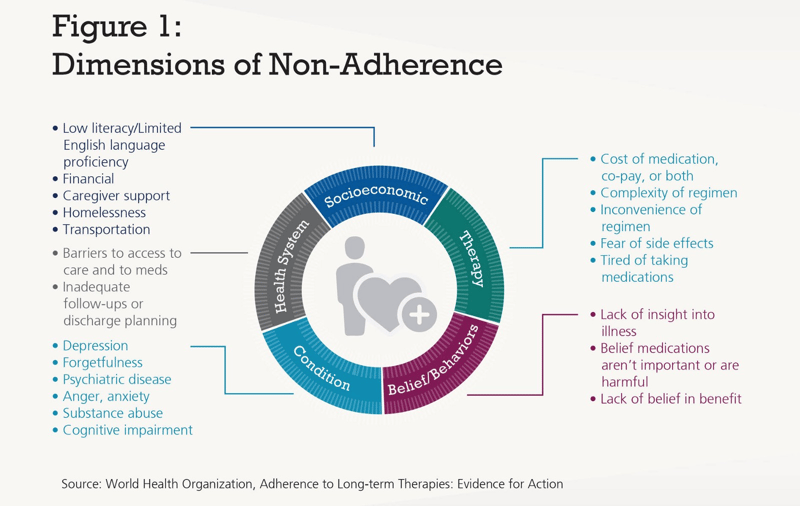
Create a full picture of each person and build personalized patient-centered care plans.
Arine approaches medication optimization comprehensively. The thousands of algorithms that make up our platform analyze clinical, social, and behavioral data and build a profile for each person. Arine's algorithms use data from readily available sources to give care teams a full picture of each person, their needs, and potential issues with their medication regimen.
The medication intelligence platform then builds a personalized patient care plan that includes recommendations and insights based on each person’s unique needs. Additionally, it translates recommendations and counseling into the individual’s language so clinicians can remove one more barrier to patient care. Each person receives personalized outreach in words that they can comprehend, enabling them to better adhere to their therapy.
Take, for instance, a person we'll call Stan who hadn’t received medication counseling in six months, despite the ten to twelve medications he takes daily. Additionally, Stan hadn’t refilled a few of his prescriptions. Arine identified the risk of a drug-related problem for Stan and triggered an outreach from his care team. Once a clinician spoke with him, they found out that he couldn’t afford his medication. The clinician reached out to the prescriber and based on Arine’s insights recommended an alternative drug covered by Stan’s insurance.
In this case, Stan was now able to afford his medication and reduce the risk of a hospital or ED visit, providing a win-win-win for all stakeholders–the health plan, the health care provider, and the individual.
Optimizing Medication Use Through Timely Interventions
Another issue in current medication management practices is finding which people need interventions and when they need them. In the past, clinical, social, and behavioral dimensions of health were seldom evaluated together and often only after an acute and serious healthcare event. This reactive approach prevented healthcare teams from identifying which people to target for medication counseling and when to intervene.
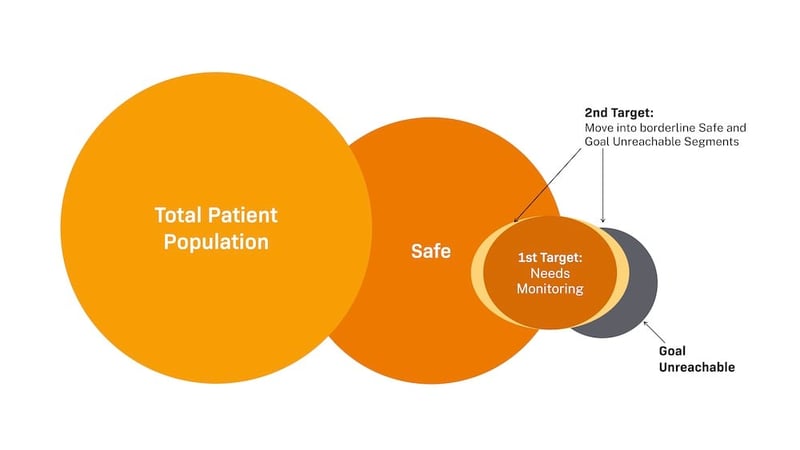
Stratify risk and choose the right population segment
The first step to delivering timely interventions to the right people is to identify people who will be the most impacted by medication counseling. Typically, we find that the best first group to target with a medication optimization program initially falls into the “needs monitoring” category. These are the people most at risk of falling out of compliance, and the segment where we can drive outcomes and decrease costs fastest. After we’ve been able to deliver measurable outcomes for this segment, we start to push outward to drive impact for people whose care goals may take longer to reach as well as to people who are on the line between medication adherence and in need of monitoring.
Identify gaps in care
Once we’ve identified people who show signs of not adhering to their medication therapy, Arine pinpoints unseen gaps in care and guides interventions for each. For instance, Arine can find people who haven’t refilled a prescription recently and guide clinicians to take action. Additionally, the platform populates smart questions for clinicians to ask each person about their medication to identify why they aren’t taking their prescriptions. Some individuals may not understand why they need the medication, and others, like Stan, may not be able to afford it.
Take another example of a person, let’s call her Lisa, who didn’t understand the many medications she was taking or why she was taking them. When our platform identified her as a person who needed extra support, a clinician was able to call and provide the education she needed to help her start adhering to her medication regimen. She felt heard and understood and finally saw why her therapy was so important. After her care team intervened, she started taking her medication and avoided more costly interventions for drug-related problems.
Medication Optimization Through End-to-End Medication Management
A key gap in medication management is end-to-end medication optimization across the care continuum. Older adults, in particular, are at risk for potentially inappropriate medication (PIM) prescribing, according to the Journal of the American Geriatric Society. Approximately 34% of adults over the age of 65 have been prescribed a PIM which costs each person on average $450 per year.
Understanding and improving care team prescribing is a critical piece to improving outcomes and reducing costs. Along with gleaning insights from a person’s data, Arine’s algorithms also analyze prescriber data. With the click of a button, care teams using Arine can deliver prescriber recommendations and track recommendation implementation in one central and collaborative dashboard.
Medication Optimization Through Customizable Solutions
When we set out to build an AI-driven medication management platform, we knew that not every population, not every health plan, and not every provider was the same, so like we personalize care to each person, each Arine client gets a customized solution for their unique and evolving needs. Everything from data inputs to care plan insights can be customized to provide your care team with the tools they need to deliver personalized care and achieve improved outcomes and decreased costs in a way that works best for your organization.
Our Medication Optimization Outcomes
Now the question remains: does Arine’s approach work? Our outcomes answer with a resounding yes. One of the exciting things about reaching a milestone like our recent round of funding is looking back on what we’ve been able to achieve up until this point. Because of our unique approach to medication optimization, we’ve made amazing strides:

What’s Next for Medication Optimization
We believe that no person should have to suffer from poor outcomes due to drug-related problems, and we believe health plans and providers can improve the costs and outcomes associated with medication mismanagement. For this reason, Arine will continue enabling safe, effective, and appropriate medication optimization to help care teams deliver outcomes at scale through medication intelligence. Stay tuned–big things are to come.
Learn more about our outcomes. Download our Quality Improvement Case Study:
Tags:
Blog Posts
October 28, 2021





Comments